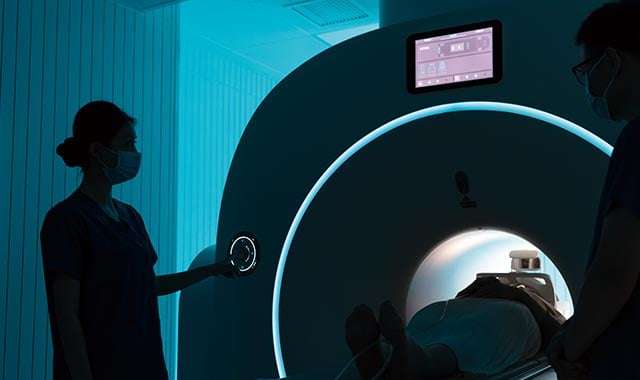
Delivering the Promise of Gene Therapy
Gene therapy has come a long way in the last ten years. In the next decade, achieving efficiencies in its delivery will unlock its full potential. Polymeric nanoparticles (PNP) show major promise as a non-viral delivery method for gene therapy.
10 Years of Evolution
CRISPR (Clustered Regularly Interspaced Short Palindromic Repeats) was discovered in 1993 as a naturally occurring acquired immune system in bacteria, for the protection against invading viral DNA. In the decade that followed, interest in this very bacteria-centric field of study grew, as researchers propelled the initial discovery of CRISPR from obscure biological research to advanced study.
In 2013, the CRISPR system was reconstituted in a test tube with its minimal necessary components, laying the foundation for a universally programable gene editor. Later that year, researchers used CRISPR for the first time in mammalian cells, demonstrating the ability to edit genomes in a completely different kingdom of life.
The decade since has brought not only a Nobel Prize1 for this discovery but also a deluge of CRISPR literature. Researchers in diverse communities around the world quickly adopted this technology, editing the genomes in organisms across the tree of life.
The impact cannot be overstated.
Continued modification has led to ongoing development and innovation, resulting in an array of powerful and precise CRISPR-based gene editors.
Most importantly, the last decade has brought CRISPR to the cusp of human gene therapy. In 2021, clinical trials conducted by both Editas and Intellia treated the very first groups of humans with CRISPR-based therapies.
In June of 2023, the FDA accepted a biologics license application (BLA) for Exa-cel,2 a CRISPR-based cell therapy to treat sickle cell disease and transfusion-dependent β-thalassemia (TDT), putting the field on track to see the first FDA approved CRISPR based therapy by 2024.
How It Works
In the simplest of terms, gene editing is the process of permanently altering the genetic material of specific cells in a living organism.
The development of CRISPR technology allows for the modification of genetic material, either through substitution, deletion, or insertion of nucleic acids, all with the intention of correcting genetic mutations.
The engine that makes gene editing possible is the DNA-cleaving protein component, that can be programmed to target specific DNA sequences.
Many “next generation” CRISPR editors have modified and improved these DNA-cleaving proteins for even more precision and efficiency, including base editors, prime editors, and CRISPR-off, to name a few. These gene editing tools allow for both the correction of genetic mutations and the precise regulation in cases where correction is too difficult.
The Hurdles
Despite these breakthroughs, the next era of gene therapy hinges on the precise delivery of the genetic payloads to their target cells or tissues.
Simply put, a viable delivery solution needs to protect the target, bind to a precise cell, cross the cell membrane, and release the cargo.
Traditionally, these payloads are administered via viral delivery methods, but several drawbacks are stunting progress.
Time and Expense
Viral delivery vehicles are difficult to mass produce, with problems including low purity and yield, resulting in expensive and inefficient manufacturing.
Low Cargo Capacity
Next-generation CRISPR therapies (such as base and prime editors) are too large to be encapsulated in a singular viral genome.
Prolonged Expression
Once genetic modifications are made, viral genomes can persist for years in the nuclei of their target cells. Over time, this continued expression can lead to off-target effects and unintended alterations.
Unintended Immunity
The body can acquire immunity to therapies in cases where multiple doses are required.
Immunogenicity
The immunogenicity of viruses may cause hepatotoxicity at doses required for effective gene therapy.
A New Method of Delivery
Polymeric nanoparticles (PNP) show major promise as a non-viral delivery method for gene therapy. PNPs could be the key to the safe and efficient delivery of a diverse range of therapeutics.
Although tiny, the nanoparticles can carry a larger payload than viral vectors. The diversity provides the potential to identify PNPs that target specific cell types, reducing unintended impacts of off-target delivery. PNPs also make repeat application possible, avoiding immunogenicity. Finally, once the intended cells are modified, the gene editing machinery naturally degrades.
Researchers at Battelle are taking PNPs one step further. They have designed a robust synthesis platform with tracking and machine learning capabilities to unlock high-throughput in vitro and in vivo screening of up to one thousand nanoparticles at a time.
Innovations like these are making it possible to go from drug to delivery system in a fraction of the time, bringing better drugs to patients faster by pairing PNPs with the next generation of CRISPR-based gene therapies.
References:
- 1The Nobel Prize in Chemistry 2020 - Prize announcement - NobelPrize.org
- 2FDA Accepts Biologics License Applications for exagamglogene… | CRISPR (crisprtx.com)
Featured Expert

Andrea McCue
Biologist III
Andrea McCue, PhD, joined Battelle’s Advanced Medicines Campaign (AMC) team as a genome engineer in November 2021. In this role, Andrea serves as a member of the non-viral gene delivery (NVGD) steering committee and is a technical lead for gene editing, while also developing and overseeing all next-generation sequencing needs for the campaign.
Before joining Battelle, Andrea completed her PhD in Molecular Genetics at The Ohio State University. She then continued her postdoctoral studies at the National Cancer Institute (Rockville, MD), and then returned to Columbus for a role as a senior researcher at The Ohio State University.
Andrea is a well-trained molecular biologist with a strong foundation of basic scientific research and over 8 years of post-PhD experience in both academic and industry research. She has a wide scientific background with specific expertise in plant molecular biology, epigenetics, gene regulation, and genome engineering.
Related Blogs
BATTELLE UPDATES
Receive updates from Battelle for an all-access pass to the incredible work of Battelle researchers.